Who is DonorConnect?
DonorConnect is the organization that connects donors with recipients. We facilitate, coordinate, educate, honor, and advocate for donors and donor families so that one day no one on a transplant waiting list dies or is limited from the lack of a life-saving organ or tissue.
Who is DonorConnect?
DonorConnect is the organization that connects donors with recipients. We facilitate, coordinate, educate, honor, and advocate for donors and donor families so that one day no one on a transplant waiting list dies or is limited from the lack of a life-saving organ or tissue.
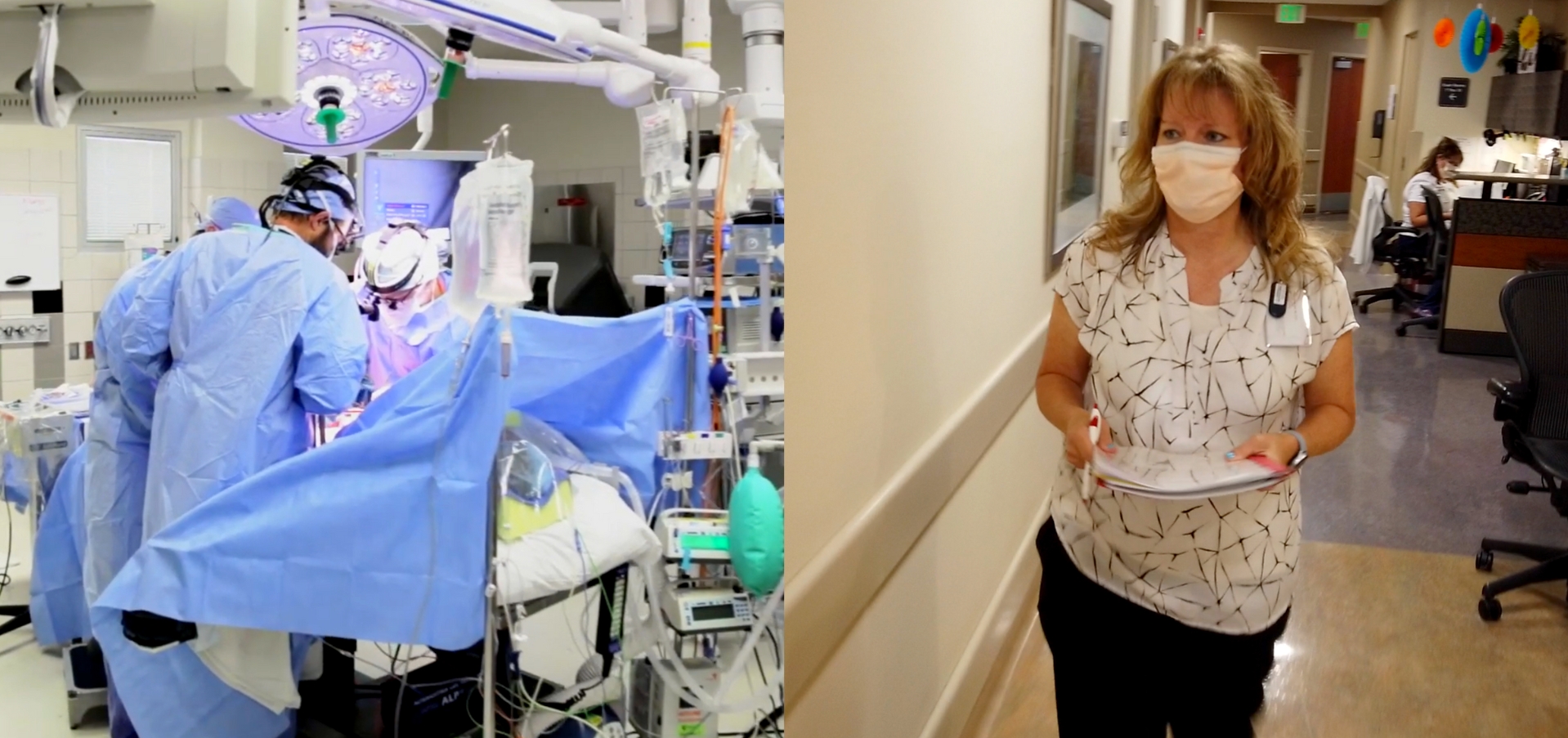
Without the organ donor, there is no story, no hope, no transplant. But when there is an organ donor, life springs from death, sorrow turns to hope, and a terrible loss becomes a gift.
Heidi’s Living Kidney Story
“I'm a little nervous about this. I'm nervous for surgery and I've got a few living donors that might come forward and they've kind of been nervous. Well, what we...
Read More
Tay Tay Tough
Three-year-old Tayzli Hale loved dancing, singing, playing with her brothers, and she loved to ride horses. Three years ago, Tayzli was thrown from her horse when an approaching car spooked the anima…
Read More
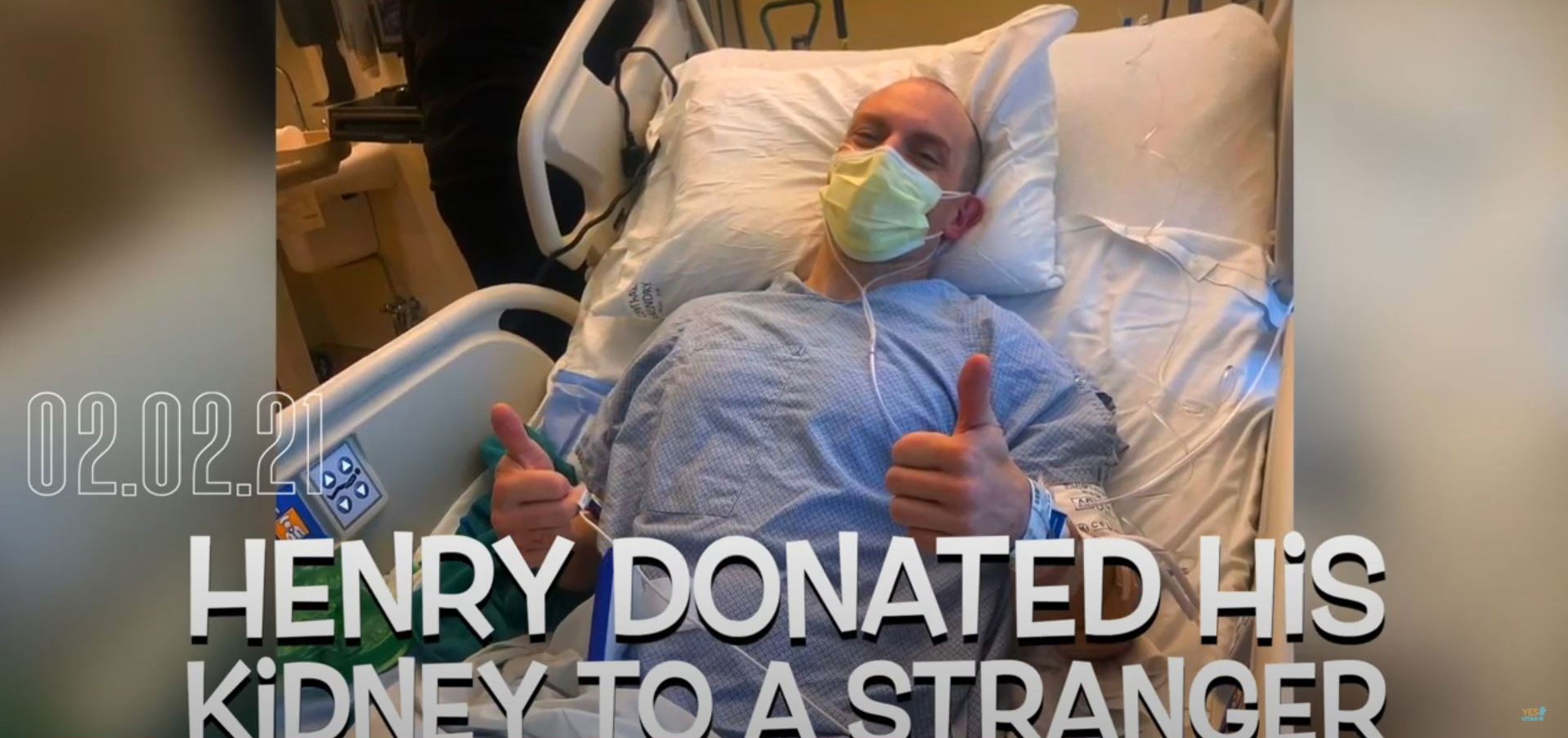
Lisa and Henry
Park City Fire District Engineer Henry Evans has run into many burning buildings to save strangers. So when his cousin went into renal failure and needed a kidney, Henry responded without hesitation. And Henry volunteered..
Read More
Every day, the generosity of donors and their families throughout the United States touches the lives of thousands of people in need.
0
Organs Donors
0
Organs Transplanted
0
Tissue and Eye Gifts
UNOS, 2021
Give Hope.Heal Life.
Support Our Life Saving Mission and Take Action
Here’s how you can get involved.
Check out the latest blogs
MLK Days of Service
Multi-cultural Outreach Specialist Rufus Tolbert had a couple of events in January where DonorConnect was able to be of service in honor of Martin Luther Kings effort to unify communities...
Read More
Kidney Donation saved my life
My name is Bruce Tippets and a kidney donation saved my life. I’m headed to the National Kidney Foundation Summit in D.C. for the second straight year, which is different from...
Read More
#shareyourspare
Living Donors make up a small portion of all organ donations. It takes a special type of person to want to donate a part of themselves to save another.
Read More